POSTPARTUM DEPRESSION IN BLACK MOTHERS: BARRIERS TO DIAGNOSIS AND TREATMENTS
Keyara Gaillard
Co-Presenters: Ugochi Adibemma, Suhavi Singh
College: College of Health Professions and Human Services
Major: BS.PUBLICHEALTH
Faculty Research Mentor: Norma Bowe
Abstract:
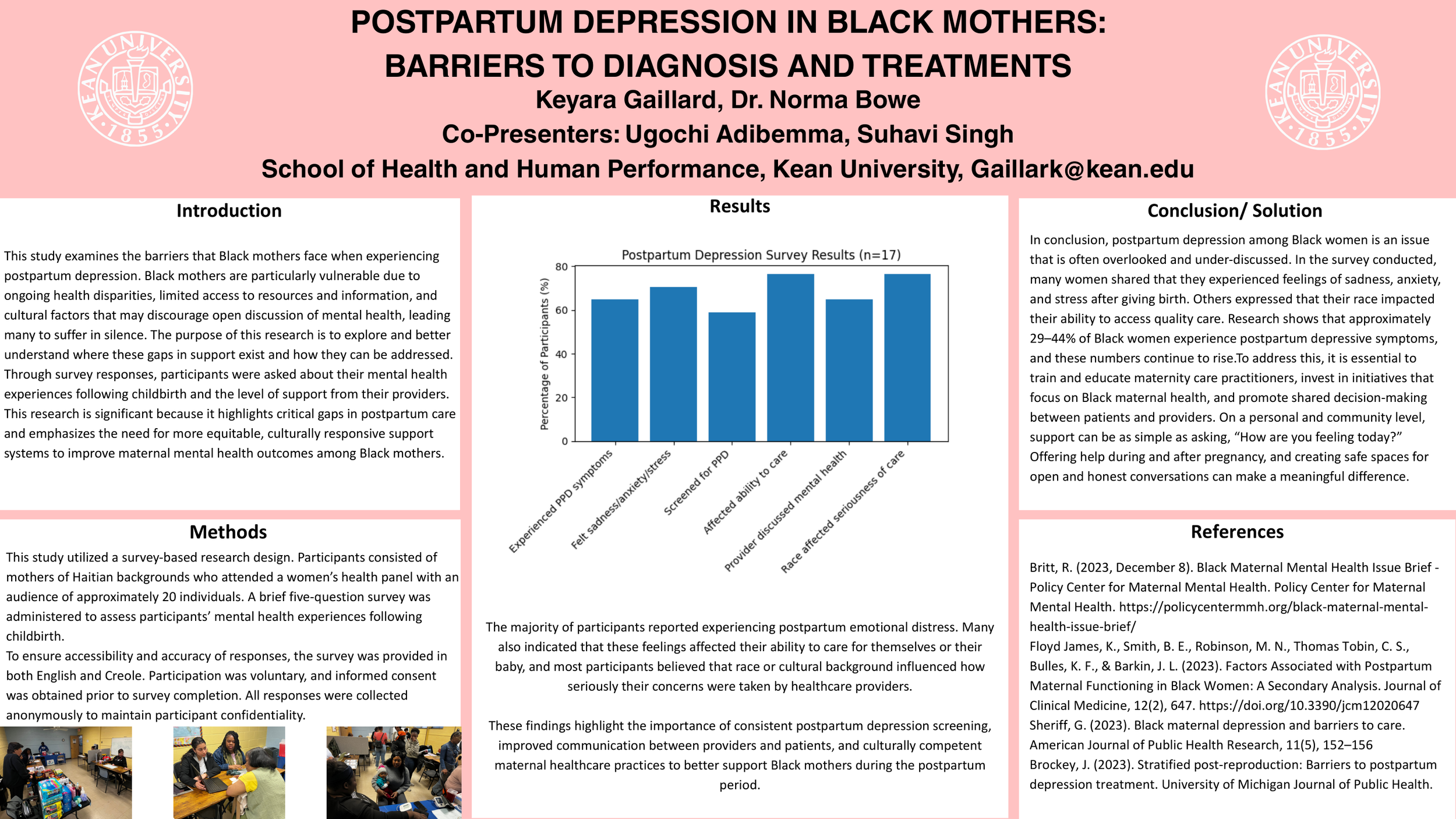
Postpartum depression (PPD) affects millions of women each year, yet its impact on Black mothers remains insufficiently recognized and inadequately addressed. Although Black women are not inherently more susceptible to postpartum depression, they are more likely to experience persistent symptoms due to systemic inequities that shape pregnancy, childbirth, and postpartum care. This project explores how structural racism, healthcare bias, and sociocultural pressures collectively create barriers to timely diagnosis and effective treatment for Black mothers experiencing postpartum depression.
One critical barrier is the inconsistency and superficial nature of postpartum mental health screening. Black mothers are less likely to be thoroughly assessed for mood disorders and more likely to have their emotional distress minimized or misattributed to stress, personality, or socioeconomic circumstances. Implicit bias within healthcare settings may influence provider perceptions, resulting in underdiagnosis or delayed referrals. Additionally, gaps in insurance coverage, transportation challenges, and limited access to culturally responsive mental health professionals reduce continuity of care beyond the immediate postpartum period.
Beyond clinical settings, cultural expectations and stigma also shape help-seeking behaviors. Narratives surrounding Black women’s strength and resilience can discourage open acknowledgment of depressive symptoms. Fear of judgment, involvement from child protective services, or being labeled as an unfit parent may further silence mothers who are struggling. These pressures are compounded by higher exposure to chronic stressors, including financial strain, workplace discrimination, and reduced access to paid maternity leave, all of which increase vulnerability to depressive symptoms while limiting time and resources for recovery.
Untreated postpartum depression has consequences that extend to infant bonding, child development, and long-term maternal health outcomes. Addressing disparities in diagnosis and treatment requires a comprehensive approach that includes extended postpartum care, culturally affirming screening practices, community-based mental health support, and policy changes that expand insurance coverage and paid leave. By reframing postpartum depression in Black mothers as a public health and equity issue rather than an individual shortcoming, this project highlights the urgent need for systemic reform grounded in reproductive justice and culturally responsive care.
