Refer or Not Refer? Assessing pediatric hematology-oncology providers’ referral practices to genetic counseling for patients with ALL/MDS/AML
Alisha Jain
Co-Presenters: Bojana Pencheva, Kelsi Hagery, Kaylee Dollerschell
College: College of Health Professions and Human Services
Major: MS.GENTICOUNSLNG
Faculty Research Mentor: Josie Pervola
Abstract:
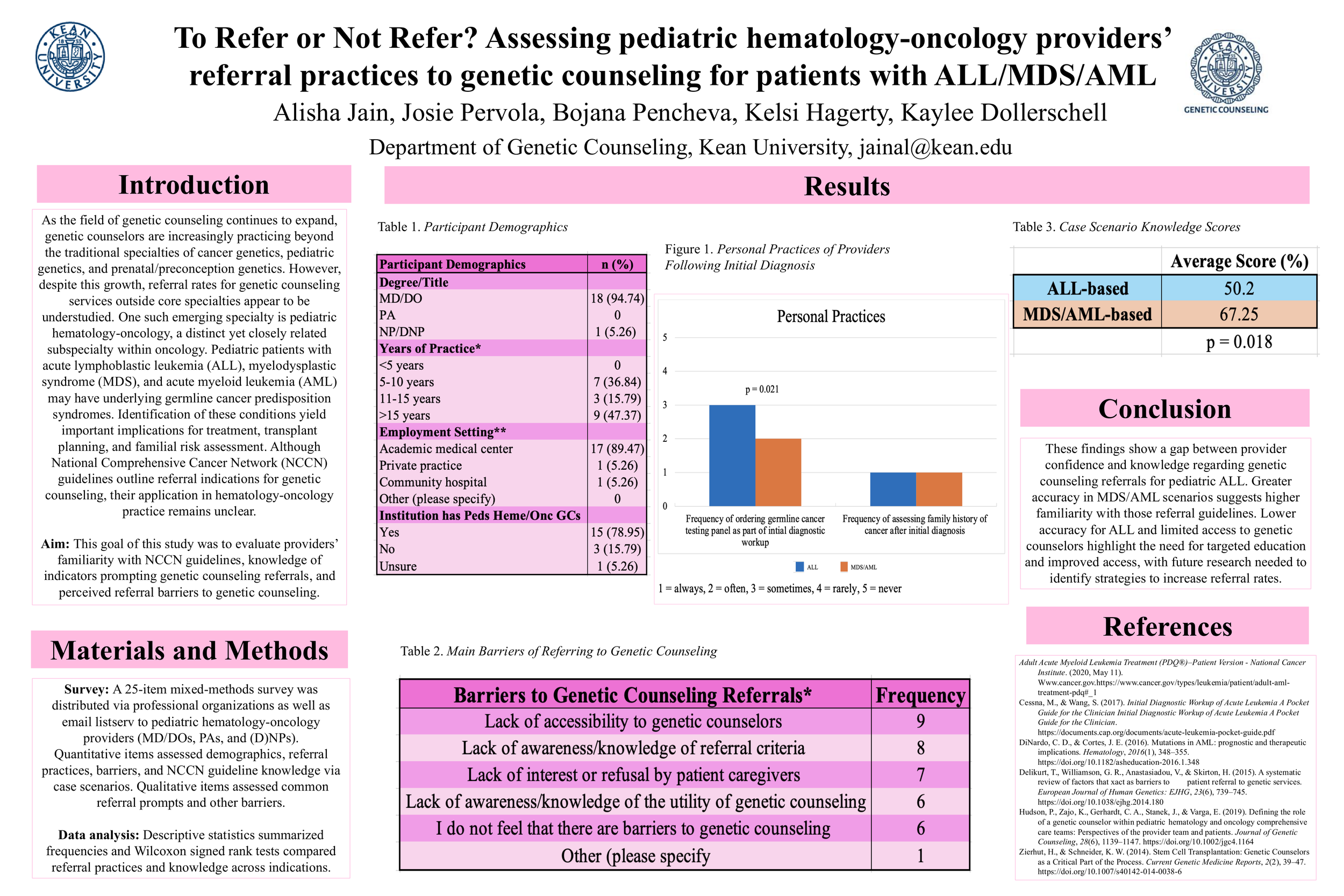
Title: To Refer or Not Refer? Assessing pediatric hematology-oncology providers’ referral practices to genetic counseling for patients with ALL/MDS/AMLAuthor: Alisha Jain, Department of Genetic Counseling, Kean UniversityIntroduction: Pediatric patients with acute lymphoblastic leukemia (ALL), myelodysplastic syndrome (MDS), and acute myeloid leukemia (AML) may have underlying germline cancer predisposition syndromes with important implications for treatment, transplant planning, and family risk assessment. Although National Comprehensive Cancer Network (NCCN) guidelines outline referral indications for genetic counseling, their application in hematology-oncology practice remains unclear.Purpose: This study evaluated providers’ familiarity with NCCN guidelines, knowledge of indicators prompting genetic counseling referrals, and perceived referral barriers to genetic counseling.Methods: A 25-item mixed-methods survey was distributed via professional organizations to pediatric hematology-oncology providers, including MD/DOs, PAs, and (D)NPs. Quantitative items assessed demographics, NCCN guideline knowledge, referral practices, and barriers. Descriptive statistics summarized frequencies and Wilcoxon signed rank tests compared referral practices and knowledge across indications. Qualitative responses were thematically analyzed to identify referral prompts and barriers.Results: Nineteen providers completed the survey. Most (79%) reported routinely assessing family history of cancer following diagnosis and expressed confidence (68%) in determining when referral was indicated based on NCCN criteria. A strong family history of cancer was the most common referral prompt for both ALL and MDS/AML patients (95%). Limited access to genetic counselors was the most prominent barrier reported (n = 9). Participants more frequently answered MDS/AML case scenario questions correctly compared to ALL scenarios (60.25%; 50.2%; p = 0.018), highlighting a gap between confidence and demonstrated knowledge, particularly for ALL.Conclusion: These findings identify a discrepancy between provider confidence and demonstrated knowledge regarding genetic counseling referrals for pediatric ALL. Greater accuracy in MDS/AML case scenarios supports the hypothesis that providers are more familiar with referral guidelines for MDS/AML than for ALL. Although family history consistently prompted referral, lower accuracy for ALL scenarios and limited access to genetic counselors highlight the need for targeted education and system-level improvements. Further research should investigate methods to improve referral rates and increase accessibility of genetic counselors in hematology-oncology.Keywords: hematology-oncology, leukemia, cancer genetic counseling, referrals to genetic counselors